- AI-Driven RCM Solution For Physicians Across The USA
End-to-End Medical Billing Company Built to Deliver Results
PRO Medical Billing Solutions is a trusted medical billing company helping healthcare providers maximize revenue and accelerate reimbursements. More than 500 providers rely on our AI-powered medical billing solutions and expert RCM support to overcome billing challenges and strengthen financial performance. Our specialists manage the entire revenue cycle, from accurate claim preparation and submission to persistent follow-ups and payment collection. The result is fewer denials, improved cash flow, and consistent revenue growth for your practice.
- No setup fees
- 100+ U.S. practices
- Specialty-focused billing team
100%
25 Days
5%


Rapid Revenue Recovery
Rejections
Electronic Payment
Client Retention
 Recovery Specialists
Recovery Specialists HIPAA Certified
HIPAA Certified 98% Claim Accuracy
98% Claim Accuracy 30% Revenue Boost Avg
30% Revenue Boost Avg 24h Turnaround
24h Turnaround 500+ US Practices
500+ US Practices AI-Powered RCM
AI-Powered RCM Denial Recovery Specialists
Denial Recovery Specialists Recovery Specialists
Recovery Specialists HIPAA Certified
HIPAA Certified 98% Claim Accuracy
98% Claim Accuracy 30% Revenue Boost Avg
30% Revenue Boost Avg 24h Turnaround
24h Turnaround 100+ US Practices
100+ US Practices AI-Powered RCM
AI-Powered RCM Denial Recovery Specialists
Denial Recovery SpecialistsNo. 1 Trusted Revenue Cycle Billing Partner
More Than a Medical Billing Company. A Partner in Revenue Growth
PRO Medical Billing Solutions is a medical billing company that follows a 2026 billing approach, unlike traditional firms still relying on outdated 1990s methods focused on claim volume rather than payment outcomes. We take a different path. Instead of counting claims, we focus on getting every claim paid by minimizing errors, preventing denials, and maximizing reimbursement opportunities.




Revenue Flow Framework
The PRO Medical Billing Solutions system is built on four foundational pillars.
forward
Pro-MBS
Process
Move claims forward without delays.
Claim Payments
That’s a common misconception; that revenue loss always means denied claims. Sometimes it comes from claims that do get paid, but not in full (underpayments).
Denial Trends
Denials feel random, but they’re not. They often follow a pattern—the same CPTs, the same documentation gaps, the same payer pushbacks.
Billing Systems
Technology isn’t the fix by itself. It’s how you use it. We use AI-backed billing systems to flag stuck medical claims, track payer turnaround times, and keep follow-ups consistent.
Why Choose Pro-MBS
We’re not coming in with a reset. We’re looking at what’s already happening.
Start with your current system
Before making any changes, we review what’s already happening and what’s getting paid. Where it slows down, where it comes back, and where claims are quietly getting stuck even when they look fine. That tells you more than any fresh setup.
We understand payer behavior
Every payer has their quirks. Some delay claims, some reduce payments quietly, while some keep asking for prescriptions, questioning whether treatment was necessary or not.
No long-term lock-ins
We never force healthcare providers into contracts because we believe if we provide good services, there is no need for one. So, our clients stay because it works, not because of a contract. If you see value, you continue. If not, you’re free to move on.
Dedicated account team
Onboarding Process
Free Audit → Custom Plan → Seamless Transition → Optimization
System Review First
We review your current billing setup, claims, and payment flow to understand how things are working today.
Data & Access Setup
We connect securely to your system and organize the data needed for clean claim handling and tracking.
Issue Mapping
We identify where claims are getting delayed, denied, or underpaid and group them by cause.
Controlled Transition
We start improving your billing flow step by step while keeping your ongoing operations stable.
Full Revenue Cycle Management Solutions
Healthcare revenue doesn’t break in one place, it leaks across coding, eligibility, authorization, billing, and follow-ups. PRO Medical Billing Solutions manages the full revenue cycle with structured workflows, payer-specific execution, and continuous claim tracking to reduce leakage, improve accuracy, and stabilize reimbursements. Every process is backed by compliance checks and measurable performance against payer behavior.
Medical Billing
We process claims with a focus on clean submission and payer-specific formatting rules, helping reduce first-pass denial rates by up to 45–77% through structured scrubbing and validation before submission.
Medical Coding
ICD-10 and CPT coding is aligned with clinical documentation to reduce coding-related denials, improving coding accuracy rates up to 96–99% through multi-layer validation checks.
Medical Credentialing
We manage payer enrollment cycles and credentialing documentation to reduce provider onboarding delays by nearly 60–80%, guaranteeing faster network participation and billing readiness.
45-Day Avg Turnaround
All Major Payers
Revenue Cycle Management
End-to-end RCM oversight helps identify leakage points across the cycle, improving overall revenue realization by 15–25% through tighter coordination between billing, coding, and follow-up.
30% Revenue Boost
Full Cycle Coverage
Accounts Receivables
98% Clean Claim Rate
< 2% Error Rate
Denial Management
Denials are categorized by root cause, coding, eligibility, authorization, or payer policy, allowing systematic reduction of repeat denials by up to 90% over time.
78% Overturn Rate
24h Response SLA
Medical Billing & Coding Audit
We conduct structured audits across claims and documentation to identify compliance gaps, coding mismatches, and underbilling opportunities, improving billing integrity scores by 25–30%
Deep Compliance Review
Actionable Reports
Prior Authorization
We manage authorization workflows with payer-specific rule mapping, reducing service delays and improving approval turnaround time by up to 30–50% depending on specialty.
Same-Day Submissions
All Payer Types
ASC Billing
Ambulatory Surgical Center billing is optimized with facility-specific coding and modifier accuracy, helping improve reimbursement capture rates by 20–35%
ASC-Certified Coders
Facility + Pro Fee
Patient Scheduling
We align scheduling with payer eligibility and procedure requirements to reduce same-day cancellations and improve appointment-to-claim conversion efficiency by 15–25%.
HIPAA Compliant
24/7 Availability
Difference Between Traditional Billing & PRO Medical Billing Solutions Revenue First Integrity Approach
- Traditional Billing
- Reacts only after denials occur, resulting in repeated CPT/ICD errors and delayed reimbursements.
- Limited control over documentation gaps, resulting in frequent payer rejections
- High AR aging due to delayed follow-ups and reactive workflows
- Revenue visibility is fragmented and inconsistent
- Weak understanding of payer behavior and rule variations
- Generic billing teams with limited specialty expertise
- No dedicated ownership of accounts, leading to repeated communication gaps
- Often locked into long-term contracts
- Higher operational cost structures
- Limited geographic and payer adaptability
- Higher risk of underpayments and write-offs due to lack of proactive audits
- PRO Medical Billing Solutions Approach
- Prevents denials through pre-submission validation and structured claim scrubbing
- Documentation-linked coding review aligned with payer-specific requirements
- Active AR management with structured follow-up cycles to reduce aging and improve recovery
- End-to-end revenue cycle tracking from eligibility to final payment posting
- Deep payer intelligence including state-wise rules and payer-specific billing logic
- Certified specialists across 200+ medical specialties
- Dedicated account managers assigned to each practice specialty
- No contracts, flexible engagement based on performance
- Transparent pricing as low as 2.49% of collections
- Nationwide coverage with state-specific payer language and compliance understanding
- Continuous audit-driven checks to protect revenue integrity and reduce leakage
Expertise Across Healthcare
Specialized billing knowledge for specialized patient care.
Orthopedic Group
Houston, TX
Aging AR and rising denial rates due to coding errors and staff turnover.
Cardiology Clinic
Dallas, TX
EHR migration caused massive billing backlog and dropped collections.
Multi-Specialty Group
Miami, FL
Unorganized credentialing causing payer rejections across 8 providers.
Dermatology Practice
Phoenix, AZ
In-house billing team missing prior auth requirements causing mass denials.
Orthopedic Group
Houston, TX
Aging AR and rising denial rates due to coding errors and staff turnover.
Cardiology Clinic
Dallas, TX
EHR migration caused massive billing backlog and dropped collections.
Multi-Specialty Group
Miami, FL
Unorganized credentialing causing payer rejections across 8 providers.
Dermatology Practice
Phoenix, AZ
In-house billing team missing prior auth requirements causing mass denials.
"Pro-MBS recovered $112,000 in denied claims we had written off. Their team is relentless, transparent, and genuinely invested in our success."
— Dr. Sarah Mitchell, Orthopedic Group, Houston TX
Pro-MBS Medical Billing Revenue Loss Calculator
See where revenue is leaking in your practice, either it’s claim refusals, underpayments, slow adjudication cycles, and missed reimbursement adjustments.
Plug-In Integration for Your EHR & Practice Management Software



















Hear from 500+ Healthcare Practices
Real results from real practices across the United States.
Get Your Instant Pricing Quote
What others charge to calculate, we give you free, see your exact billing cost in minutes, no strings attached.
Texas
South Central
Cardio
ASC
Oncology
Ortho
Active — Serving Texas
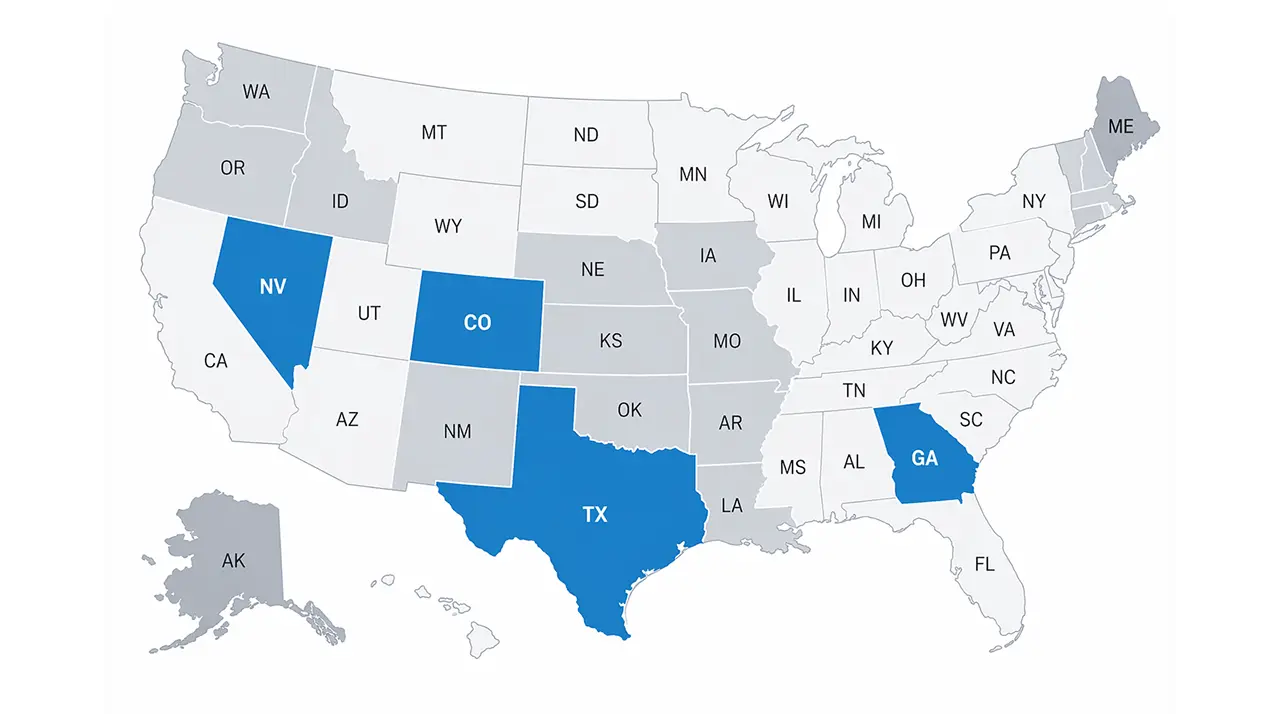
All 50 States Covered
Nationwide Coverage
As a top-leading medical billing company, our reach spans across the USA, supporting healthcare practices with state-wise payer rules, localized billing understanding, and consistent operational expertise.
See What Changes Once PRO Medical Billing Solutions Takes Over
InternalCare
Internal medicine group reduced preventable denials and improved collections in 90 days
Read the case study
CardioPlus
A cardiology practice recovered aging AR with payer-specific denial appeals
Read the case studye
Internal Medicine
Internal medicine group reduced preventable denials and improved collections in 90 days
Read the case studye
CarioVesuclar
A cardiology practice recovered aging AR with payer-specific denial appeals
Read the case studye
Office Locations
PRO Medical Billing Company uniting expertise and tech to meet your vision
Thousands of providers are growing their practice with PRO Medical Billing Solutions, a trusted medical billing company. Now it’s your turn.
Nationwide Support
Connecting healthcare providers with reliable medical billing expertise across multiple office locations.
Let's Talk Revenue
Our billing specialists are ready to analyze your practice and show you exactly how much revenue you can recover.
Free 30-Minute Practice Consultation
No commitment. We’ll analyze your billing data and show you exactly where you’re losing revenue.
Send Us a Message
Frequently Asked Questions
Answers to the questions we hear most from practice administrators.
Get a Free Billing & Coding Audit Now
Optimize your medical billing workflow. Fill out the form and our team will contact you within 24 hours.
